TMS Therapy in Kenosha: A Guide for Treatment-Resistant Depression
Blog:TMS Therapy in Kenosha: A Guide for Treatment-Resistant Depression
TMS Therapy in Kenosha: A Guide for Treatment-Resistant Depression
Most people who try antidepressants get some relief. But a meaningful percentage — studies suggest somewhere between a third and half of patients with major depressive disorder — do not respond adequately to medication alone, even after trying more than one. If that has been your experience, you have likely heard the phrase "treatment-resistant depression" at some point. It is a clinically accurate term, but it can also feel like a door closing rather than opening.
TMS therapy is one of the options that exists specifically for that situation. It works through an entirely different mechanism than medication, which is precisely why it can succeed where antidepressants have not. This post explains what TMS is, how it works, what the treatment process actually looks like, and what realistic expectations for outcomes should be — so that if you are considering it, you have a clear picture before you make any decisions.
What Treatment-Resistant Depression Actually Means
Before getting into TMS specifically, it helps to understand what "treatment-resistant" means clinically, because the term is sometimes used loosely. In most clinical contexts, treatment-resistant depression refers to major depressive disorder that has not responded adequately to at least two different antidepressant medications at appropriate doses and duration.
That distinction matters for a few reasons. First, it rules out cases where medication may not have had sufficient time to work, or where the dose was too low. Second, most insurance coverage for TMS is tied to this threshold — meaning the documentation of prior treatment attempts is typically a prerequisite for approval.
Treatment-resistant depression is not rare. And its persistence is not a reflection of the patient's effort or mindset. Depression involves measurable changes in brain chemistry and circuit activity, and those changes do not always respond to the same interventions in the same way across different people.
How TMS Works
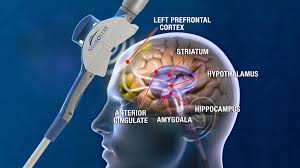
Transcranial Magnetic Stimulation (TMS) uses brief, targeted magnetic pulses to stimulate nerve cells in specific regions of the brain involved in mood regulation — primarily the left dorsolateral prefrontal cortex (DLPFC), an area that tends to show reduced activity in people with depression.
Pulses are delivered via a coil placed against the scalp. They are similar in strength to the pulses used in MRI machines, though localized to a much smaller area. Over the course of a full treatment cycle, repeated stimulation of the underactive circuit gradually restores more normal patterns of activity. The mechanism differs from that of medication, which works systemically through neurotransmitter pathways — which is one reason TMS can be effective even when medications have not been.
TMS is non-invasive and does not require anesthesia, sedation, or any downtime. There are no systemic side effects of the kind associated with antidepressants — no weight changes, no sexual side effects, no cognitive blunting. The most common side effects are mild scalp discomfort or a headache during or shortly after the session, which typically lessen over the first week of treatment as patients become accustomed to the sensation.
A Ray of Hope in Kenosha uses the BrainsWay Deep TMS system, which is FDA-cleared for major depressive disorder. You can learn more about our TMS services and the technology we use here.
What to Expect During a Treatment Course
The standard TMS protocol for depression involves five sessions per week for approximately six weeks, for a total of around 36 sessions. Each session lasts 20-40 minutes, depending on the protocol used. Patients sit in a reclined chair, a technician positions the coil against the scalp, and the session proceeds with a series of pulses that produce a tapping or clicking sensation at the treatment site.
There is no recovery time required. Most patients drive themselves to and from appointments and return to normal activities — work, errands, exercise — immediately afterward.
Improvement typically does not appear all at once. Many patients begin to notice changes in sleep, energy, or motivation around weeks three or four, with mood following somewhat later. For others, changes are more gradual, and the full benefit is not apparent until the course is complete or even a few weeks afterward. This variable timeline is worth knowing in advance, because it affects how to interpret early sessions that may feel unremarkable.
Our TMS technicians in Kenosha guide patients through every session, track responses over the course of treatment, and communicate regularly with the psychiatry team. That coordination matters — TMS at A Ray of Hope is not a standalone intervention; it happens within the context of ongoing psychiatric care.
What the Research Shows
Response rates for TMS in treatment-resistant depression are consistently better than what most patients expect, particularly given that they've already tried other options without success. Across clinical trials and real-world data, roughly 50 to 60 percent of patients with treatment-resistant depression experience a meaningful reduction in symptoms following a full course of TMS. Approximately 30 percent achieve full remission — a complete resolution of depressive symptoms.
Those numbers compare favorably to the likelihood of achieving remission from a third or fourth antidepressant trial, which drops significantly with each prior medication failure. TMS does not work for everyone, and it is important to approach it with that honesty intact. But for a patient who has tried multiple medications and is still struggling, it represents a genuinely different pathway with real evidence behind it.
The durability of response is also worth noting. Patients who respond to TMS tend to maintain improvement for months to a year or longer. Some eventually need a second course of treatment — often a shorter one — if symptoms return. Ongoing psychiatric support, including therapy and medication management when appropriate, helps sustain improvement over time. You can learn more about the full range of mental health conditions we treat at A Ray of Hope here.
Who TMS Is Appropriate For
TMS is generally a good fit for adults with major depressive disorder who have not achieved adequate response from at least two antidepressant trials. It may also be considered for patients who want to avoid antidepressants entirely due to side effect history or personal preference, provided the clinical picture supports it — though insurance coverage in those cases is less predictable.
There are a small number of contraindications. TMS is not recommended for patients with implanted metallic devices in or near the head (cochlear implants, certain aneurysm clips, deep brain stimulators), or for those with a personal history of seizures or epilepsy. Pregnancy is a relative consideration that requires individual evaluation.
TMS is not a replacement for therapy or psychiatric care. It is most effective when it is part of a broader treatment plan that addresses the psychological and behavioral dimensions of depression alongside the neurological. Our mental health providers and psychiatry team work alongside the TMS program to support patients through the full course of treatment.
Starting the Conversation in Kenosha
If you have been struggling with depression and have not found adequate relief from medication, TMS is worth a serious conversation with a psychiatrist. It is not a last resort — it is an FDA-cleared, well-researched treatment that works through a different mechanism than what you have tried before.
A Ray of Hope offers TMS therapy at our Kenosha location at 4600 Green Bay Road. Because TMS requires a clinical evaluation and prior authorization from insurance before starting, the process begins with a psychiatric consultation. To start that process, reach out to our team directly — you can contact us here or call (847) 816-6335. For general information about our Kenosha office, visit our Kenosha location page.
Frequently Asked Questions
How is TMS different from electroconvulsive therapy (ECT)?
TMS and ECT are both brain stimulation treatments, but they work differently and have very different profiles. ECT uses electrical current and requires general anesthesia, and is typically reserved for the most severe or acute cases of depression. TMS uses magnetic pulses, requires no anesthesia or sedation, has a milder side effect profile, and is appropriate for a broader population of patients with treatment-resistant depression.
Can I continue my current medications during TMS?
In most cases, yes. TMS is frequently used alongside ongoing medication management or therapy rather than as a replacement. Your psychiatrist will review your current regimen and make recommendations based on your individual situation.
Does TMS hurt?
Most patients describe the sensation during TMS as a tapping or light knocking at the treatment site. Some experience mild scalp discomfort or a headache in the first several sessions. These side effects typically diminish significantly by the end of the first week as patients acclimate to the treatment.
If you or someone you care about has been searching for TMS near me or wondering whether treatment-resistant depression has other options, A Ray of Hope in Kenosha is here to help you work through those questions. Call us at (847) 816-6335 or reach out online to get started.




